Mid Cycle (coding)
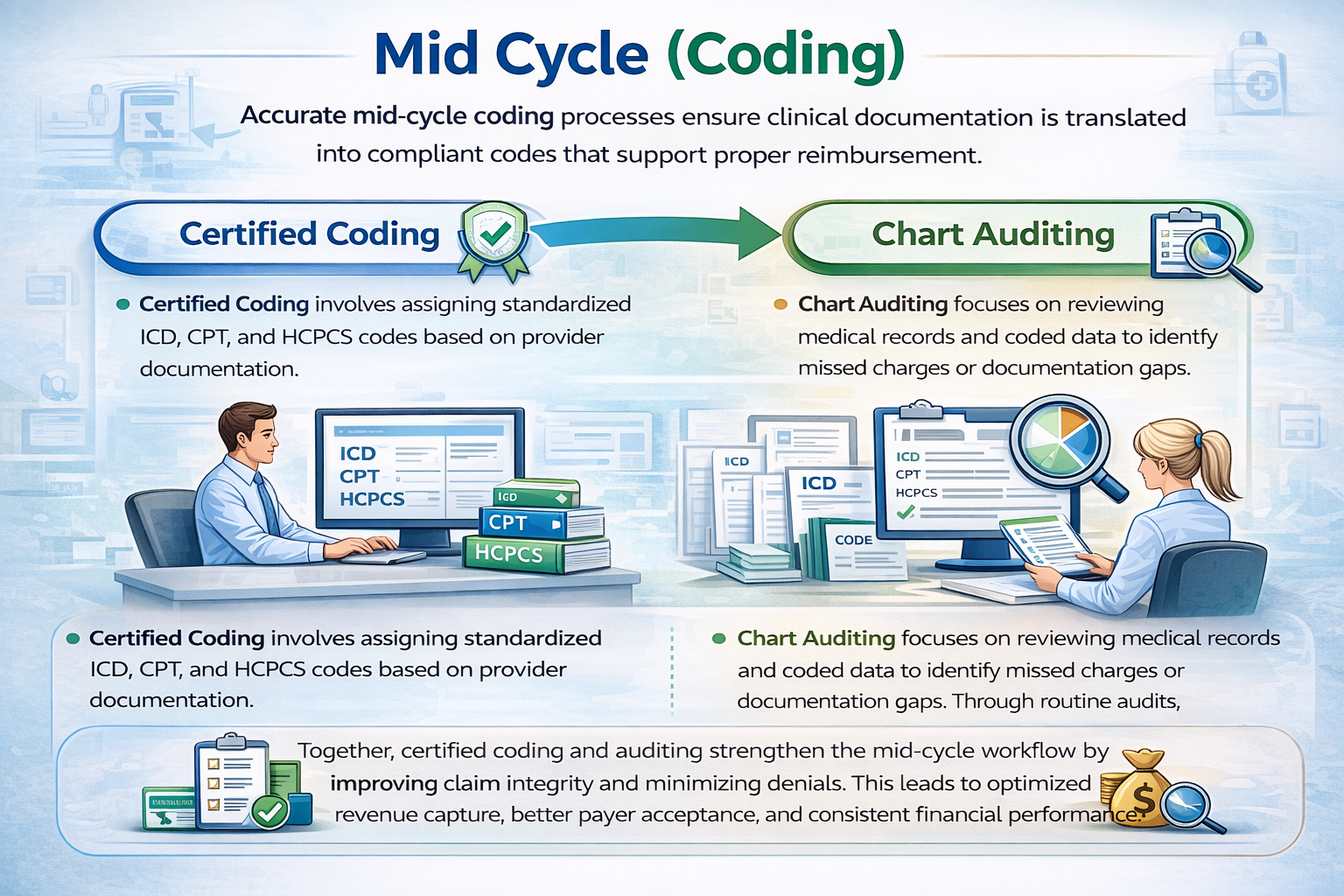
Accurate mid-cycle coding processes ensure clinical documentation is translated into compliant codes that support proper reimbursement.
Certified Coding involves assigning standardized ICD, CPT, and HCPCS codes based on provider documentation. This ensures claim accuracy, regulatory compliance, and appropriate payment for services rendered.
Chart Auditing focuses on reviewing medical records and coded data to identify missed charges or documentation gaps. Through routine audits, organizations can enhance coding quality, reduce compliance risks, and capture full revenue potential.
Together, certified coding and auditing strengthen the mid-cycle workflow by improving claim integrity and minimizing denials. This leads to optimized revenue capture, better payer acceptance, and consistent financial performance.