Front End
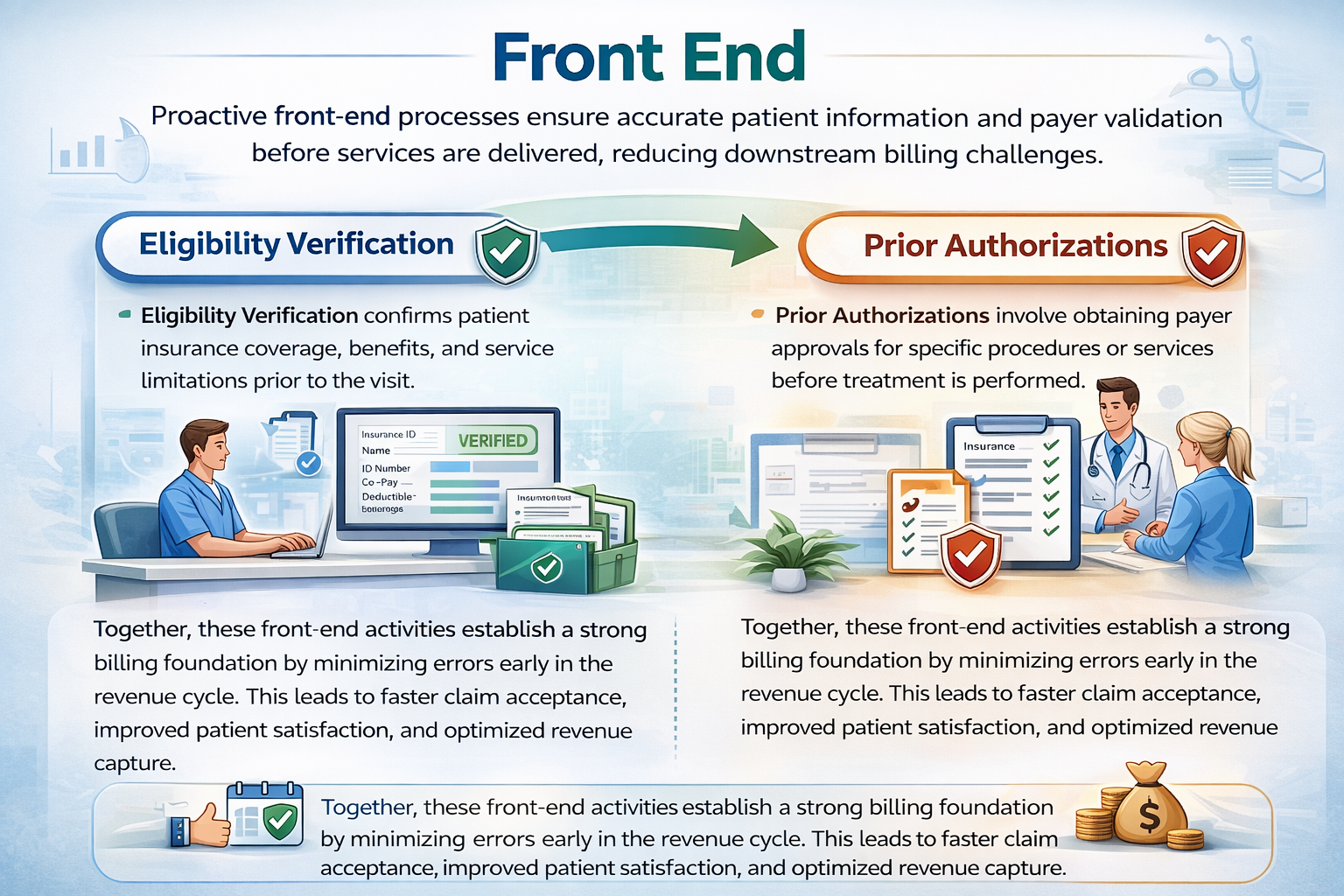
Proactive front-end processes ensure accurate patient information and payer validation before services are delivered, reducing downstream billing challenges.
Eligibility Verification confirms patient insurance coverage, benefits, and service limitations prior to the visit. This helps prevent claim rejections, improves transparency, and ensures smoother reimbursement workflows.
Prior Authorizations involve obtaining payer approvals for specific procedures or services before treatment is performed. By securing authorization in advance, providers avoid medical necessity denials and unexpected payment delays.
Together, these front-end activities establish a strong billing foundation by minimizing errors early in the revenue cycle. This leads to faster claim acceptance, improved patient satisfaction, and optimized revenue capture.