Back End
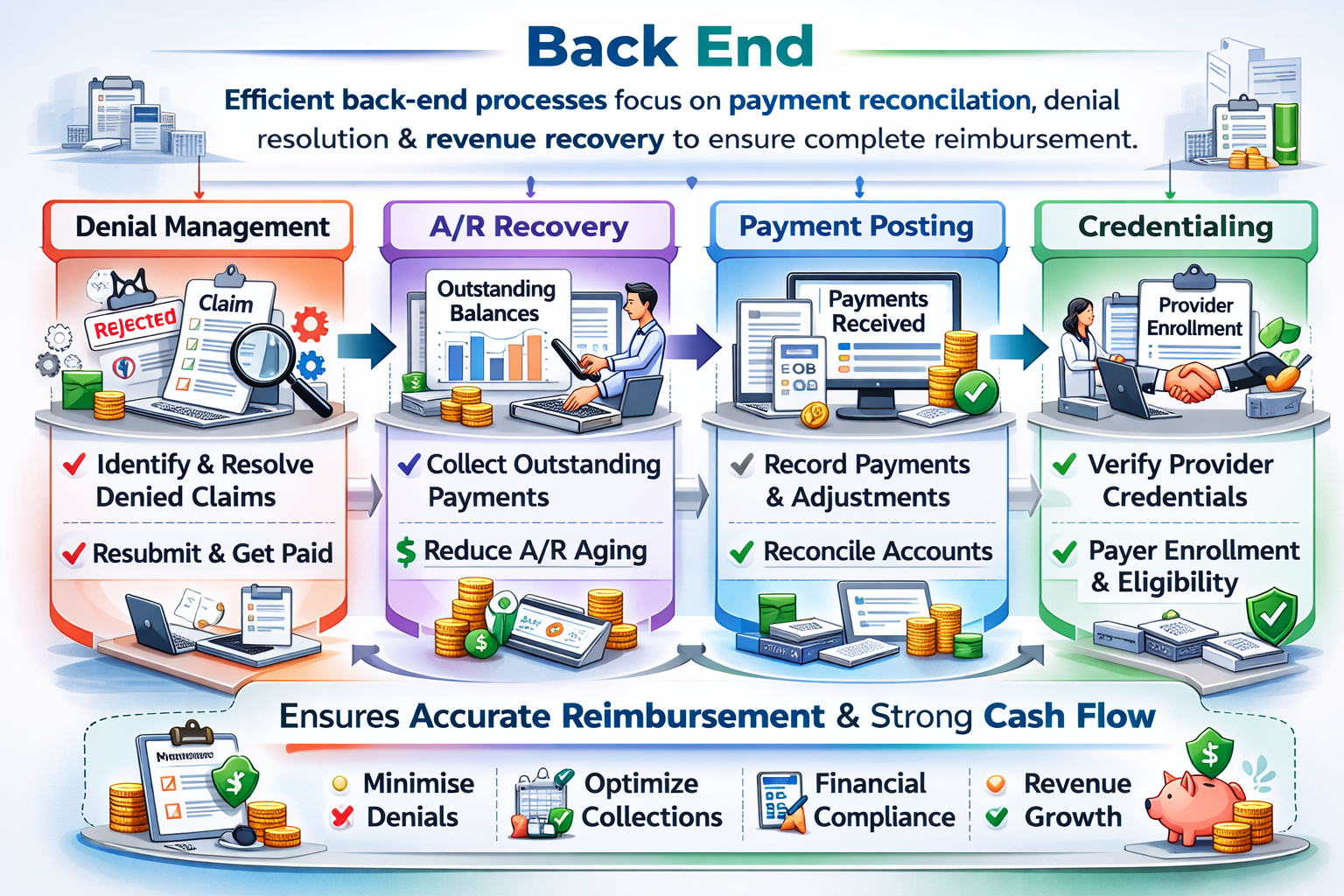
Efficient back-end processes focus on payment reconciliation, denial resolution, and revenue recovery to ensure complete reimbursement.
Denial Management involves identifying, analyzing, and correcting rejected claims to enable timely resubmission and payment. A/R Recovery focuses on following up with payers and patients to collect outstanding balances and reduce aging receivables.
Payment Posting ensures accurate recording of insurance and patient payments, adjustments, and contractual write-offs. This process maintains financial transparency and supports effective revenue tracking and reporting.
Credentialing verifies provider qualifications and enrolls them with payers to enable claim submission and reimbursement eligibility. Together, these back-end activities strengthen cash flow, minimize revenue leakage, and sustain financial performance.